Neurosurgery
Preventative health
Preventative medicine to us is more than just identifying all your risk factors and working to mitigate them. It’s also getting to know our patients thoroughly, so we know when things aren’t quite right and establishes trust and understanding between us. The importance of this cannot be overstated.
Prevention comes in many forms, from the simplest things we do every day such as sleep and what we eat, to being more active with both intentional and incidental exercise.
Immunisations, travel advice and vaccinations, cancer screening (cervical, breast and bowel), age specific health checks, sexual health checks and skin checks are great examples where we put prevention into action.
It’s in our logo and we strongly believe in the power of Preventative Healthcare.
At GS Health we encourage new patients to book in for at least a 30-minute initial consultation. This allows us to get some extra information about your family history in detail, your personal history, and look at some risk factors for chronic disease.
If you have substantial medical history, then 45 minutes is encouraged.
If you absolutely need to just pop in for a cold, we’re happy to accommodate you, but encourage coming in again when you’re well to go over things in more detail. From then on, we know you well and everything is a much easier fix!
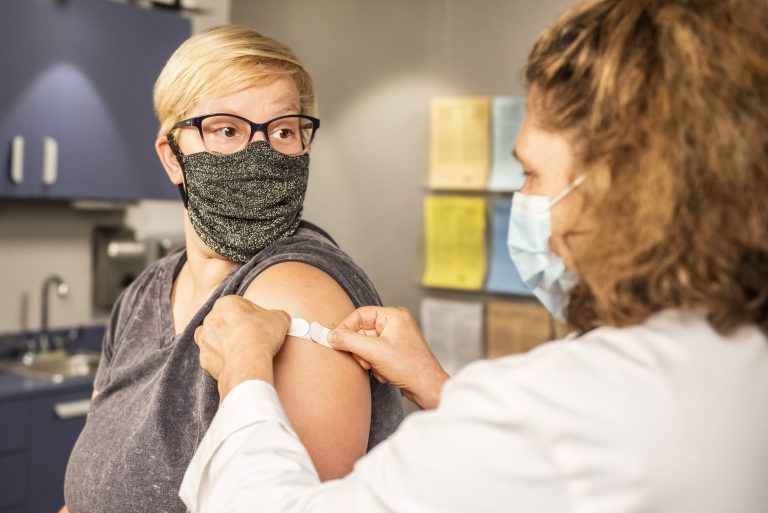
Immunisations are an excellent form of preventative healthcare with vast amounts of research performed into the safety and effectiveness of each vaccine. The routine schedule of vaccinations provides good protection for people living and working in Australia, but some conditions that are less common are not covered.
An example of this is (Bexsero) meningococcal B, which is increasing in prevalence since we’ve done such an excellent job in reducing meningococcal C in Australia.
It may eventually become part of the government schedule, but at present is available as a private vaccine, and available at GS Health.
Certain groups at particular risk can receive vaccinations funded by the commonwealth government or the NSW government in the form of catch, and these are stocked at GS Health. Please visit our catch up vaccinations page for more information.
http://www.health.nsw.gov.au/immunisation/Pages/gp_catchup.aspx
Seasonal influenza immunisation is also available at GS Health and covers 4 strains. Having had the worst influenza season on record in NSW (and guys, trust me it was a bad one), we highly encourage anyone who can receive the vaccination to get it.
Employers can also arrange vaccinations for their employees, and if there are enough of you, we can visit your workplace. Visit our workplace vaccinations page or contact us for more information.
If you’re after vaccinations before you head away, rest assured you’re in good hands. Visit our travel health page for more information on the suggested vaccinations for your destination.
Travel planning and advice is critical particularly for more adventurous travel (which comes with adventurous activities and eating) and making sure your health is well covered before stepping out of your comfort zone.
We owe many lives to the sacrifice of Mrs Papanicolaou for what is now a commonplace screening test. Dr Georgios Papanikolaou (and Dr Aurel Babeș not long before him) had discovered that by examining the cells of the cervix, they could see if any cancerous or precancerous cells were visible.
We’ve come a very long way since 1923, and from the 1st of December 2017 the pap smear has been replaced with a more sensitive and more specific test known as the Cervical Screening Test (CST).
So, what are we testing for?
With the new cervical screening test, a sample from the cervix is tested for the HPV virus itself which is the precursor to most changes. If there is no virus, then the test will be conducted in another 5 years. If the test is positive for HPV, the cells in the sample are examined in a laboratory for abnormal changes.
If abnormal cells are present, the abnormality is graded into low- or high-grade changes, and your doctor will chat to you about what happens next. These changes are not diagnostic of cancer, but mean we’ll need to do repeat cervical screening sooner or arrange for further testing to clarify what’s going on.
Who should get a cervical screening test?
Anyone with a cervix who has ever had sex (this includes male to female, and female to female sex) or skin to skin genital contact, are recommended to undergo cervical screening.
When should I get a cervical screening test?
Cervical screening starts from the age of 25, though earlier in some circumstances. If the test is negative for HPV your next test will be in 5 years.
If your last test was before the 1st of January 2018, it’s likely you had a pap smear. Your first cervical screening test is 2 years after your last pap smear.
In order to collect a good sample and reduce the chance of requiring a repeat test, it’s best to wait until your period has finished to organise your cervical screening test.
What happens if the result is abnormal?
An abnormal result does not necessarily mean you have cervical cancer. Most HPV infections clear up on their own without any need for treatment. A positive HPV test means the cells are looked at closely under the microscope.
In a small number of women these changes can progress to high-grade abnormality. And in an even smaller number of women persisting high-grade changes may progress to cervical cancer.
However, 80% of cervical cancers are detected in women who have never had a pap smear or haven’t been having regular screening.
An abnormal result means another test is often required, which may be a repeat cervical test at a shorter interval, or some further tests via a gynaecologist.
What about the HPV vaccine?
The HPV vaccine has been an amazing discovery that Australia can very proudly call a homegrown success story. And while the HPV can reduce the risk of contracting some high-risk types of HPV, it doesn’t protect against all causes of cervical cancer, hence why regular screening is still an important step in prevention.
Often, it’s difficult for someone to know what skin condition they have, because they all look and feel so similar. Red, dry, itchy. So why bother knowing what they are?
Because the long-term management of all the different skin conditions (and there are thousands) can be quite different. But the most commonly seen skin conditions in general practice is eczema and dermatitis, so read on for more information and some great tips to help get them under control.
If you’re on an internet surfing session, check out Dermnet NZ or the Australian College of Dermatology A-Z of skin. Don’t be too tempted to pattern match, as I said there’s a lot of red itchy skin conditions out there.
Eczema/Dermatitis
The terms eczema and dermatitis are often used interchangeably, which confuses a lot of people. Dermatitis is inflammation of the skin, specifically the epidermis layer. Eczema is another name for the same thing, though it’s common that people refer to eczema when they mean atopic dermatitis.
And to complicate things further, the duration and site of the dermatitis often gives it different names.
Atopic dermatitis
This is the type of dermatitis often seen in younger children and babies and there is a h2 inherited component. Often a parent or sibling also has either dermatitis, asthma, or hay fever (allergic rhinitis) or all three. It’s fairly uncommon in children under 4 months old, although there are other similar looking skin conditions that can occur at this age.
The skin becomes easily irritated, usually involving the cheeks in very young children, the outside of joints (front of knees, backs of elbows) in toddlers and preschoolers, later involving the inside of joints in children as they age (inside the front of the elbow or behind the knees).
As adults get older the eczema can become very localised and very thick, sometimes causing darkening of the skin.
Irritant contact dermatitis
This form of dermatitis is caused by either physical or chemical irritation to the skin, causing damage faster than it can be repaired.
The commonest irritants are water, soaps, detergents, solvents, acids, adhesives, and friction.
Commonly found in professions where a lot of contact with chemicals or regular hand washing occurs like hairdressers, medical staff, food preparation, nail technicians and factory workers.
Young children learning to eat can have irritation from dribble that comes out the mouth onto the skin, or from a nappy that might have been left on too long whilst full. Also, people who lick their lips will get irritation of the surrounding skin.
One thing not to forget is that cosmetics can cause an irritant contact dermatitis, even after prolonged use with no issues. In patients with rosacea for example, as the underlying condition worsens the cosmetics can irritate further.
Allergic contact dermatitis
While it may seem similar to irritant contact dermatitis, allergic contact dermatitis differs in its mechanism and onset.
It’s a delayed type of hypersensitivity reaction, causing a rash about 48-72 hours after contact with a specific allergen. It is different to getting a rash after ingestion of an allergen and can develop to something you’ve been in contact with all your life.
Common reactions are to adhesive bandages, watch bands, certain gloves, cosmetics, acrylate glue from nail cosmetics, and nickel in jewellery.
Sometimes an allergic reaction only occurs after contact has been made AND the area gets exposed to UV light (sunlight). This is called photo-contact dermatitis
Discoid eczema (nummular dermatitis)
Triggered off by trauma to the skin, like injuries or insect bites, discoid eczema is so called because of its round or oval shape. It can also be triggered by generally dry skin, contact dermatitis, or other skin issues.
It is often mistaken for ringworm because of the similar shape and appearance, and if there are only one or two lesions some scrapings might need to be taken to clarify the diagnosis.
It appears to affect males more than females but affects children and adults equally.
Dandruff and Seborrhoeic Dermatitis
Seborrhoeic dermatitis is a very common type of eczema/dermatitis that affects the gland rich areas of the scalp, face and trunk. As such people find inside the hair, beard and armpits can become quite inflamed.
Dandruff is the name we give to the uninflamed version. This is also called pityriasis capitis. This produces flakes of dry skin in the hair bearing areas of the scalp.
We’re not completely sure what causes it, but can be associated with a proliferation of Malassezia, a type of yeast that usually resides on the skin.
Infantile seborrhoeic dermatitis (or cradle cap) usually occurs in babies younger than 3 months old but resolves by 12 months of age.
Adult seborrhoeic dermatitis starts in late teenage years and is associated with.
- Oily skin
- Family history
- Lack of sleep or stressful events
- Immunosuppression: People with organ transplants or immunodeficiency syndromes
- Neurological conditions
Adults typically experience the following.
- Worsening in winter – improving in summer
- Minimal itching most of the time
- Combination facial skin (oily and dry)
- Scaly red eyelids (blepharitis)
- Flakey patches on the hairline or anterior chest
- Rash in armpits, under the breasts, in the groin folds or genital creases
- Inflamed hair follicles on the cheeks and upper body
Otitis externa (dermatitis)
Otitis externa means inflammation of the external ear canal. The passage between the outside world and the ear drum.
Usually, we see these as infections following an injury (scratches from fingernails) or use of cotton buds to clean, or following swimming where water gets trapped in the canal and irritates.
However, it is possible to get dermatitis in the ear also, for people that suffer from any of the above types of dermatitis.
Symptoms include itchy ears, dry skin coming out of the ear canal, sometimes crusting and an ooze, and pain.
Other forms of dermatitis
There’s also venous eczema associated with varicose veins, gravitational eczema associated with swollen legs, and a Mayerson naevus which is eczema that involves moles.
Treatment strategies
Although some of the specific types of dermatitis require specific treatment, there are general principles that all follow that will prevent recurrence and improve the symptoms.
Avoidance of triggers
If you know that springtime brings about a flare up in your asthma, hayfever AND your dermatitis, then being prepared will help avoid the flareup being worse. Using a daily antihistamine and vacuuming regularly can make things better.
If you have allergic contact dermatitis, then make sure you don’t allow yourself to come into contact with those triggers.
Bathing
Avoid taking baths too often. The prolonged exposure to warm water can cause the skin to dry out after and cause microtears making it easy for the skin to become irritated. Showers are better, and even then, the shower should be as cool and short as you can tolerate.
For example, wet the body, turn the water off, use a non-soap cleanser (such as QV wash or Cetaphil), then turn the water on to rinse, and voila, end of shower.
Clothing
Clothes that are coarse and irritating can trigger eczema. Things like wool, or clothing that doesn’t breathe are often worse.
Moisturising and emollients
Keeping the skin hydrated is essential, and the use of a non-irritating moisturiser daily is very helpful in preventing flares. To simplify this step using a wash that is moisturising can help. Again, QV wash, Cetaphil wash are some good non irritating products. You can ask your pharmacist for help selecting an appropriate wash.
Sometimes when the skin is very dry you might need a h2er emollient, something quite thick that really holds the moisture in. Dermeze and urederm 10% are both very potent, without added fragrances.
Topical steroids
Although there is a lot of fear about prolonged topical steroid usage, it is often the opposite which causes the most problems – ineffective usage or inadequate treatment. Steroids come in varying strengths from very mild over the counter steroids typically for the face, to very h2 steroids in a fatty base for persisting thick eczema.
This is important to get right, so chat to your doctor and make sure you are clear on how to use it, how much to apply, how often and for how long.
Non steroid anti-inflammatory cream
There are new creams that work very well for eczema/dermatitis without the side effects of steroids but are quite expensive. They are cheaper on the PBS for patients suffering eczema around the eyes, or those who have conditions where steroid usage can make things worse. It is possible to get this on a private prescription if your doctor feels there is a benefit in it.
Bleach baths
For patients with eczema and dermatitis all over the skin, where colonisation with staphylococcus aureus is an issue, then reducing the load of bacteria improves the recurrence of flares.
Fill up a bathtub by measuring how many 10L buckets it takes to fill. Place the bucket under the tap and pour it into the bath keeping count.
Then add
- 1-2 capfuls of bathoil
- 100g (1/3cup) of pool salt for each 10L of water
- 12mL of White King Bleach (4% bleach) per 10L of water
This is then performed for.
- Every day for 1 month
- Three times a week for 1 month
- Once a week for 1 month
- Stop when the eczema settles
You can either recommence or increase the frequency if the eczema begins to flare again.
If you are worried that your eczema isn’t being well controlled, or you would like to know ways to improve, book in with your doctor at GS Health.
Most new parents are aware of the NSW Blue Book (or the personal health record) and all the frequent checks to make sure bubs are growing up healthy and well.
As a reminder the checks are at.
- 1-4 weeks of age (usually 2)
- 6-8 weeks (with immunisations)
- 4 months (with immunisations)
- 6 months (with immunisations)
- 12 months (with immunisations)
- 18 months (with immunisations)
- 2-year check
- 4-year check (with immunisations)
Of course, we encourage check-ups at any stage if parents have concerns about their child’s development.
What most people don’t know is there are checks at older ages to ensure chronic disease is identified earlier and often prevented.
40–49-year-old diabetic health assessment.
People in this age bracket are encouraged to complete the AUSDIAB questionnaire, which is designed to stratify diabetes risk into low, medium and high. Check it out with this link.
If you score 12 or more, and are a regular patient of GS Health, we encourage you to book in with our nurses and doctors for a comprehensive health assessment. This service is bulk billed and can be conducted every 3 years between 40-49 years of age if eligible.
45–49-year-old health check for adults at risk of developing a chronic disease.
People in this age group with a risk of developing a chronic disease are encouraged also to attend for a comprehensive health check. Eligibility includes but is not limited to.
- Lifestyle risk factors, such as smoking, physical inactivity, poor nutrition or alcohol use.
- Biomedical risk factors, such as high cholesterol, high blood pressure, impaired glucose metabolism or excess weight; and
- A family history of a chronic disease
If you do qualify, our nurses will conduct a comprehensive health assessment looking at clarifying your risk factors and suggesting ways to reduce your risk of developing any chronic diseases.
This is eligible to be bulk billed once in this age group.
Annual health assessments
The following groups are entitled to annual health assessments to ensure the time is given to thoroughly assess the risk factors that lead to chronic disease and manage and improve activities of daily living.
- People aged 75 years or over
- Permanent residents of aged care facilities
- People with an intellectual disability
One off health assessments
A special one-off health assessment that isn’t dependant on age is available for groups that do need to catch up on their health.
- People aged 75 years or over
- Permanent residents of aged care facilities
- People with an intellectual disability
If you have any questions at all about health assessments and if you need one, please don’t hesitate to give us a call.
The doctors at Green Square Health are able to provide a comprehensive skin check, give the most up to date information on skin protection, and if necessary, use the best equipment to remove anything suspicious for examination in a certified laboratory.
What to expect from a skin check with your doctor
- You will be asked about your personal history and family history with skin cancers, your occupational history, any previous excisions, history of sun exposure and frequency of sun protection
- In order to examine you carefully, we will need to expose as much skin as possible. The rooms are set to allow for maximal privacy, so please wear underwear you are comfortable in. you will be provided with a gown or sheet to allow us to inspect different areas at a time
- You should let the doctor know which lesions you are most concerned about
- If you are concerned about a skin lesion on your scalp, or that is covered by underwear, please let the doctor know so we can examine these areas with your consent
What should I look out for?
- New moles that you have never noticed before
- Moles that increase in size over time
- An outline of a mole that becomes notched or irregular
- Change in colour on a spot from brown to black, or has varied colours through it
- A spot that develops a lump within it or becomes raised above the normal skin level
- Rough, scaly or ulcerated surfaces begin to develop
- Moles that itch or tingle
- Moles that bleed or weep
- Spots that look different from your other spots
How can I prevent skin cancer?
Slip on clothes that cover as much skin as possible
- Wear shirts with collars when out in the sun, arm protectors when cycling, and a rashie or wetsuit when in the water or surfing
Slop on some sunscreen
- SPF30+ filters out 97% of UV radiation, however it only works if enough is used and it’s used properly (Use SPF50+ if possible)
- put it on before you leave home, at least 20 minutes before sun exposure and reapply every 2 hours (this is what most people forget)
- put it on even more regularly if you’ve been swimming or sweating a lot
- try waterproof sunscreen if you can
- put it everywhere the sun touches, both arms and legs, front and back of the body, on your face, neck, ears, hands and feet
Slap on a hat
- something wide brimmed to protect your face, back of the neck, eyes and ears
Seek some shade
- 11am-3pm is when the sun and its UV rays are strongest, so try to make sure you have a shady spot especially during those hours
Slide on your fashionable sunnies
When choosing something you imagine wearing on a beautiful coastal walk, or sipping a coffee at your favourite alfresco café, make sure it will provide adequate protection from UV rays.
- See if they meet the Australian Standard AS/NZS1067:2003
- Look for the words ‘good UV protection’ on the label, and look for categories 2, 3 or 4. These block 95% of UV radiation
- Some sunglasses have an eye protection factor or EPF rating. EPF 9 or 10 exceed the Australian Standard and block almost all UV radiation
- Check they are suitable for driving
- Polarised sunglasses reduce glare and can make it easier to see on a sunny day, see through reflective water surfaces, or make it easier to notice small objects on road glare if cycling
- The Australian Standard for sunglasses does not cover prescription glasses. Some prescription glasses provide UV radiation protection – check with your optometrist.
Associated links